Pet Health Resources
Please click on a pet health topic below to learn more. If you have any questions after reviewing the topic, please contact us to schedule a consultation with one of our veterinarians.
Choosing a Diet
Choosing a Diet
What diet should I choose for my pet?
There are a number of good commercial diets on the market. Our animal hospital sells Science Diet and Royal Canin, although there are many others that are acceptable. Keep in mind that the laws governing pet food companies are minimal. Here are a few things to look for:
• High quality protein sources at the top of the ingredient list.
• Whole grains are ideal. Avoid products that contain corn, cornmeal, corn derivatives (other than corn gluten meal), or soy derivatives at the top of the ingredient list, as they are generally thought of as cheap fillers, and commonly aggravate allergies. Other cheap fillers include “soybean mill run”, “soy flour”, “oat groats”, “wheat gluten”, among others. Remember that these names, as they pertain to pet food, do not have the same meaning as in human foods.
• Avoid products that contain “meat byproducts” or “animal byproducts” (not specifying which kind) or “meat byproduct meal”. Whenever an animal protein source is not specific, manufacturers can include the flesh of any animal. This can include, among other disturbing ingredients, rendered animals from agricultural operations.
• Also, avoid byproducts where possible. Whenever you see the word “byproduct”, this is defined as any part of an animal not fit for human consumption. Byproducts are not meat; they are essentially everything BUT meat. There are diets on the market that contain no animal byproducts of any kind. Brands include Nutro, Wellness, Naturapet, Merrick, and Chicken Soup for the Pet’s Soul, among others. Look for “human grade” where possible.
• Avoid price brands sold at discount stores. Often these diets contain so many cheap fillers, your pet will have to eat a higher quantity to be full, so the “deal” may not even be that fabulous.
• Individual needs vary, so please check with our animal clinic for the best recommendation for your pet, or if you have any further nutritional questions.
Choosing a diet for your pet can be stressful. There are numerous “boutique” brands on the market with beautiful bags and wonderful sales pitches. It can be difficult to wade through the information and know what to feed your pet! Our veterinarians recommend Royal Canin, Hill’s Science Diet, or Purina. We feed our own animals these foods and we investigate carefully what goes into these diets and the ethical standards of these companies. Please contact our veterinary team to discuss your pet’s individual dietary needs.
Helpful links for more information on choosing a diet for your pet:
• Committee Nutrition Global WSA: Recommendations on Selecting Pet Foods
Declawing
Declawing
Is it cruel to have my cat declawed?
Our veterinarians do not recommend declawing your cat. Declawing can be very stressful and can cause further aggression and litterbox problems. We encourage training kittens to allow their paws to be handled at a young age, making nail trims much easier into adulthood. Additionally, our veterinarians recommend keeping scratching posts in each room of the house. Try using different materials, i.e. carpet, wicker, cardboard, etc, and try some that lay flat on the floor and some that stand up and down. Cat’s usually favor one material or another. If your cat is exhibiting destructive scratching, please contact our animal clinic for a behavioral consultation.
Dental Health
Dental Health
I was totally unaware that dogs and cats have dental problems. Is it common?
Dental disease is the most common disease in dogs and cats. Over 68% of all pets over the age of three have some form of periodontal or dental disease. Some pets will show few signs of dental disease. It is up to the pet’s family and veterinarian to uncover this hidden and often painful condition.
Are dental problems the same in pets and people?
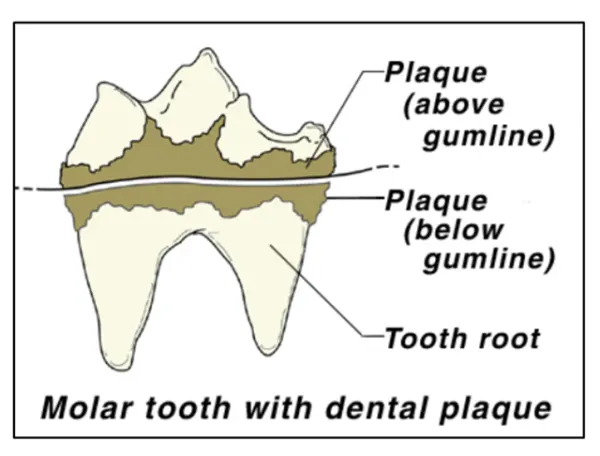 No. In man the most common problem is tooth decay which, due to the loss of calcium from the enamel, results in painful infected cavities. In dogs, decay represents less than 10% of dental problems. The majority of dental disease in dogs and cats is periodontal disease.
No. In man the most common problem is tooth decay which, due to the loss of calcium from the enamel, results in painful infected cavities. In dogs, decay represents less than 10% of dental problems. The majority of dental disease in dogs and cats is periodontal disease.
What is periodontal disease?
Periodontal disease is inflammation or infection of the tissues surrounding the tooth. Accumulation of tartar (calculus) on the teeth and under the gum contributes to gum recession around the base of the tooth, and infection soon follows. Untreated infection then spreads into the tooth socket and ultimately the tooth loosens and is lost. Infection can also spread to other organs in the body such as the heart valves, kidneys, and liver.
Is periodontal disease very common?
It is estimated that over 68% of dogs over three years old suffer from some degree of periodontitis, making it by far the most common canine disease.
What is tartar and can it be prevented?
The mouth of all mammals is home to thousands of bacteria. Many of these bacteria will breed on the surfaces of the tooth and form an invisible layer called plaque or biofilm. Some of this is removed naturally by the dog’s tongue and chewing habits but if allowed to remain the plaque thickens, becomes mineralized and is then visible as tartar (calculus). The tartar presses on the gums, which recede, and the bacteria then result in gum inflammation and infection (gingivitis). The gums continue to recede until ultimately the socket is infected and the tooth is lost.
As the oral infection increases tonsillitis and pharyngitis can also occur. In addition, the bacteria are absorbed into the blood stream and can be carried to other organs. Heart valve infections (endocardiosis or endocarditis), kidney and liver problems are frequently due to bad teeth.
Can tartar be prevented?
 Plaque is mineralized in some dogs and cats much quicker than others. Special toys as well as feeding the newer dental diets help reduce tartar build up, as does regular home care – tooth brushing. Tooth brushing is the single most important prevention for dental disease. Today there are many products designed to reduce tartar in our pets.
Plaque is mineralized in some dogs and cats much quicker than others. Special toys as well as feeding the newer dental diets help reduce tartar build up, as does regular home care – tooth brushing. Tooth brushing is the single most important prevention for dental disease. Today there are many products designed to reduce tartar in our pets.
Will feeding dry food remove tartar?
Once tartar has formed it will be necessary to remove it with a professional scaling and polishing under anesthesia. There are exciting new dental diets that can help reduce the formation of plaque and tartar in your pet.
What is involved with a dental cleaning for my dog?
The goal of dental scaling and polishing is to remove the tartar and invisible plaque. We will perform pre-anesthesia blood tests to ensure that kidney and liver function are satisfactory. Sometimes antibiotic treatment is instituted before full dental prophylaxis is carried out. Our veterinarians will be happy to discuss this with you.
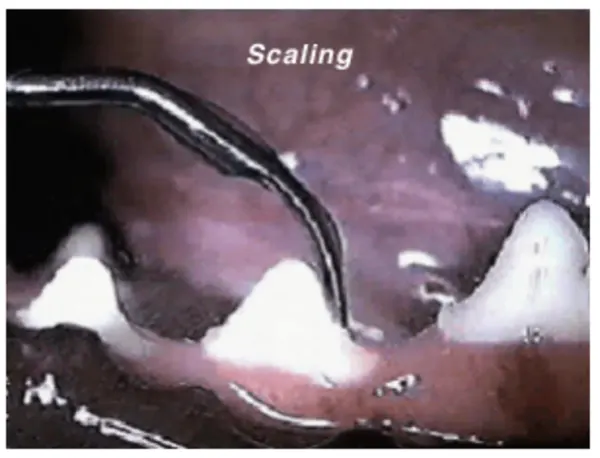
Tooth scaling will be performed both by hand and using ultrasonic cleaning equipment to remove tartar both above and below the gum line. The tartar beneath the gum line causes the most significant gum recession. The teeth are then polished in order to help prevent or minimize subsequent plaque build-up. It may be necessary to carry out other procedures at the same time such as extractions and special applications such as fluoride may be indicated to decrease tooth sensitivity and strengthen enamel.
These procedures will be fully discussed both before your pet’s dental cleaning and when you bring your pet in for the procedure. We will need a telephone number where you can be reached during the dental cleaning so that we can discuss any additional work that may be indicated once we begin.
Do I have to make an appointment for my dog to have a scale and polish?
Yes. Our veterinary team will perform pre-anesthesia blood tests and examine your pet for any other underlying disorders.
How can I prevent tartar accumulation after the procedure?
 Plaque and tartar begin forming in as little as six hours after your pet’s dental cleaning. We recommend beginning a home dental care program for all pets. We will provide you with detailed instructions on how to brush your pet’s teeth.
Plaque and tartar begin forming in as little as six hours after your pet’s dental cleaning. We recommend beginning a home dental care program for all pets. We will provide you with detailed instructions on how to brush your pet’s teeth.
Can I use human toothpaste?
Do not use human dentifrice or toothpaste on any account. These are foaming products and are not meant to be swallowed. Additionally, many types of human toothpaste contain sodium, which may cause problems in some pets.
Dental information is based on material written by Ernest E. Ward Jr., DVM.
©Copyright 2002 Lifelearn Inc. Used with permission under license.
Fleas
Fleas
Pet owners should be concerned with only one species of the over 2000 species of fleas, Ctenocephalides felis, the cat flea. This is the flea that we find on our pets (cats, dogs, rabbits, and other species) in 99.9 percent of cases.
Fleas can cause serious health problems for you and your pet.
Fleas aren’t just a nuisance! Fleas can kill our pets!
Fleas suck blood leading to blood loss and anemia. A heavy flea burden is lethal, especially to smaller or younger animals. The cat flea has even been known to kill animals as large as dairy calves through heavy infestation.
Fleas can transmit infections and parasites
Fleas can carry and transmit a bacteria called Bartonella that can cause health issues in cats, dogs, and people. Fleas can carry a type of parasite, called Dipylidium caninum (tapeworm) that can suck nutrients from the pet’s intestine and cause anal itching.
Fleas can cause serious skin issues
Fleas can cause severe itching and also other problems such as skin infections and hair loss. Some animals can become allergic to fleas, and flea allergy dermatitis is the most common skin disease of dogs and cats. Our veterinarians see far too many patients for this condition when routine, high quality flea control could have saved much pain and suffering on the pets part.
 Common Myths
Common Myths
Even though fleas are the most common parasite in dogs and cats, there are many misconceptions about them. Myths that veterinarians hear about fleas almost every day are:
Myth: My pet cannot have fleas because he lives entirely indoors.
Fact: Fleas thrive particularly well in the well-regulated temperatures in the home. We hear this a lot when it comes to indoor cats!
Myth: My pet cannot have fleas because if there were any fleas they would be biting me.
Fact: The cat flea, Ctenocephalides felis, can suck the blood of a wide variety of animals. However, this flea definitely does not prefer human blood and won’t eat it unless absolutely necessary. Humans tend not to be bitten unless flea population numbers are high.
Myth: We do not have fleas because we only have hard wood floors.
Fact: Fleas love to develop in the cracks between the boards of hard wood floors.
Myth: My pet cannot have fleas because I would see them.
Fact: You cannot expect to see fleas because many animals will lick, groom, and chew after being bitten by a flea, especially cats. This causes the flea to either jump off the pet or get swallowed.
 The Flea Life Cycle
The Flea Life Cycle
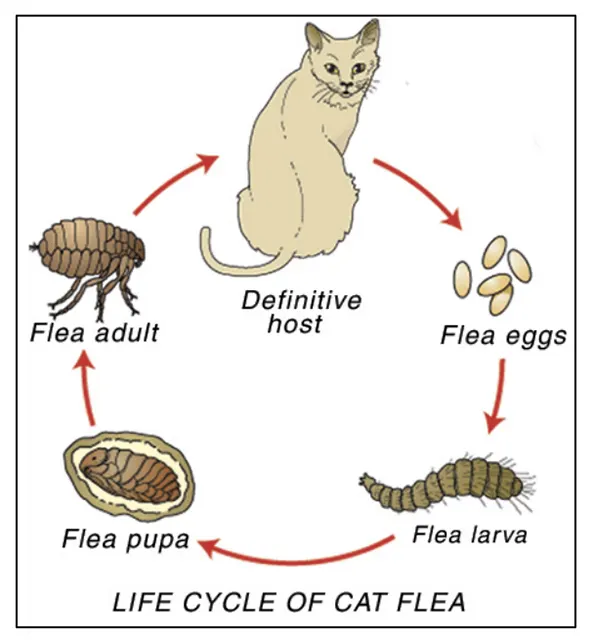
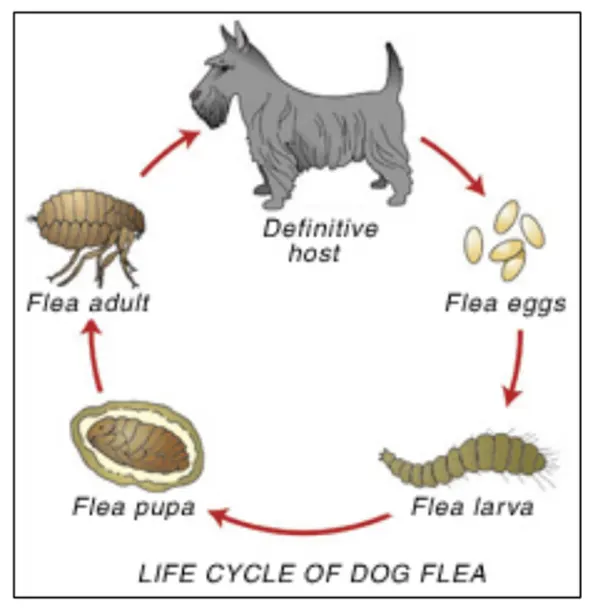
There are four life stages of the flea. For effective flea control, it is important to know how to break this life cycle in more than one place.
The flea life cycle consists of egg, larval, pupal, and adult stages. Eggs are laid in the hair coat and are designed to fall off your pet and into your home. Larvae hatch from the eggs and develop in a pet’s environment by feeding on adult flea feces (i.e. digested blood) that fall out of the hair coat of the pet. Larvae eventually spin cocoons, often within carpet fibers, for pupation. Pupae are resistant to freezing, drying, and insecticides, and can lie dormant for many months! New fleas develop from pupae and can begin feeding within hours of finding a dog or cat. The entire flea life cycle can be completed in as little as three weeks.
Flea Control Strategies
New Products
Today, veterinarians have some great flea control products in our arsenal. There are now many effective and safe new products to choose from. Please call our pet clinic for recommendations!
Break the Flea Life Cycle
A two-step approach, targeting both the adult flea and the egg or larval flea forms, provides the most rapid control and the least resistance to flea control agents in future flea generations.
Year-round Flea Control
Fleas are also adaptive and the temperature controls how fast the flea completes its lifecycle. If you want to eradicate the flea population in a specific home, it is best to attack when numbers are low in the winter. Stopping flea control products in the winter may make it much harder to gain the upper hand in the spring and summer when the populations are rising.
Information courtesy of The Veterinary Dermatology Consults
Heartworm
Heartworm
What causes heartworm disease?
Heartworm disease (dirofilariasis) is a serious and potentially fatal disease in dogs and cats. It is caused by a blood-borne parasite called dirofilaria immitis.
Heartworms are found in the heart and adjacent large blood vessels of infected animals. The female worm is 6 to 14 inches long (15 to 36 cm) and 1/8 inch wide (5 mm). The male is about half the size of the female. One dog may have as many as 300 worms.
How do heartworms get into the heart?
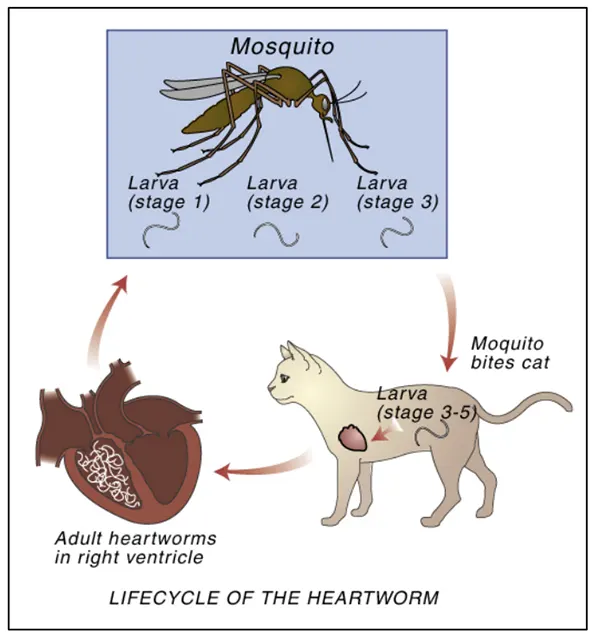 Adult heartworms live in the heart and pulmonary arteries of infected animals. They have been found in other areas of the body, but this is unusual. They live up to five years and, during this time, the female produces millions of offspring (microfilaria). These microfilariae live mainly in the small vessels of the bloodstream. The immature heartworms cannot complete their life cycle in your pet. The mosquito is required for some stages of the heartworm life cycle. The microfilaria are not infective (cannot grow to adulthood) in the body — although they do cause problems.
Adult heartworms live in the heart and pulmonary arteries of infected animals. They have been found in other areas of the body, but this is unusual. They live up to five years and, during this time, the female produces millions of offspring (microfilaria). These microfilariae live mainly in the small vessels of the bloodstream. The immature heartworms cannot complete their life cycle in your pet. The mosquito is required for some stages of the heartworm life cycle. The microfilaria are not infective (cannot grow to adulthood) in the body — although they do cause problems.
As many as 30 species of mosquitoes can transmit heartworms. The female mosquito bites the infected pet and ingests the microfilariae during a blood meal. The microfilariae develop further for 10 to 30 days in the mosquito and then enter the mouthparts of the mosquito. The microfilariae are now called infective larvae because at this stage of development, they will grow to adulthood when they enter an animal. The mosquito usually bites the dog/cat where the hair coat is thinnest. However, having long hair does not prevent a dog from getting heartworms.
When fully developed, the infective larvae enter the bloodstream and migrate to the heart and adjacent vessels where they grow to maturity in two to three months and start reproducing, thereby completing the full life cycle.
Where are heartworms found?
 Canine heartworm disease occurs all over the world. In the United States, it was once limited to the south and southeast regions. However, the disease is spreading and is now found in most regions of the United States and Canada, particularly where mosquitoes are prevalent.
Canine heartworm disease occurs all over the world. In the United States, it was once limited to the south and southeast regions. However, the disease is spreading and is now found in most regions of the United States and Canada, particularly where mosquitoes are prevalent.
How do animals get infected with them?
The disease is not spread directly from animal to animal. An intermediate host, the mosquito, is required for transmission. Spread of the disease therefore coincides with mosquito season. The number of animals infected and the length of the mosquito season are directly correlated with the incidence of heartworm disease in any given area.
It can take a number of years before pets show outward signs of infection, depending on severity. Consequently, the disease is often diagnosed mostly in four to eight year old dogs. The disease is seldom diagnosed in a dog less than one year of age because the young worms (larvae) take five to seven months to mature after infection.
What do heartworms do to the body?
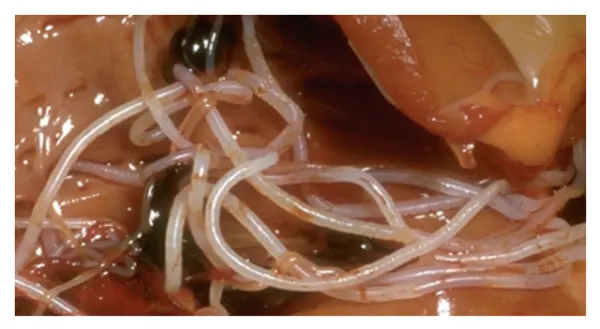
Adult heartworms: Adult heartworms cause disease by clogging the heart and major blood vessels leading from the heart. They interfere with the valve action in the heart. By clogging the main blood vessels, the blood supply to other organs of the body is reduced, particularly the lungs, liver and kidneys, leading to malfunction of these organs.
Dogs and cats infected with heartworms may not show any signs of disease for as long as two years. Unfortunately, by the time clinical signs are seen, the disease is well advanced. The signs of heartworm disease depend on the number of adult worms present, the location of the worms, the length of time the worms have been present, and the degree of damage to the heart, lungs, liver, and kidneys from the adult worms and the microfilariae.
The most obvious signs are a soft, dry cough, shortness of breath, weakness, nervousness, listlessness, and loss of stamina. All of these signs are most noticeable following exercise, when some dogs may even faint.
 Listening to the chest with a stethoscope will often reveal abnormal lung and heart sounds. In advanced cases, congestive heart failure may be apparent and the abdomen and legs will swell from fluid accumulation. There may also be evidence of weight loss, poor condition, and anemia. Severely infected pets may die suddenly during exercise or excitement.
Listening to the chest with a stethoscope will often reveal abnormal lung and heart sounds. In advanced cases, congestive heart failure may be apparent and the abdomen and legs will swell from fluid accumulation. There may also be evidence of weight loss, poor condition, and anemia. Severely infected pets may die suddenly during exercise or excitement.
Microfilariae (Young heartworms):
Microfilariae circulate throughout the body but remain primarily in the small blood vessels. Because they are as wide as the small vessels, they may block blood flow in these vessels. The body cells being supplied by these vessels are deprived of the nutrients and oxygen normally supplied by the blood. The lungs and liver are primarily affected.
Inflammation of lung tissue leads to coughing. Cirrhosis of the liver causes jaundice, anemia, and general weakness because this organ is essential in maintaining a healthy animal. The kidneys may also be affected and allow poisons to accumulate in the body.
How is heartworm infection diagnosed?
In most cases, diagnosis of heartworm disease can be made by a blood test that can be run in the veterinary hospital or by a veterinary laboratory. Further diagnostic procedures are essential to determine if the dog can tolerate heartworm treatment. Depending on the case, we will recommend some or all of the following procedures before treatment is started.
Serological test for antigens to adult heartworms: This is a test performed on a blood sample. It is the most widely used test because it detects antigens (proteins) produced by adult female heartworms. It will be positive even if the dog does not have any microfilaria in the blood. This occurs in about 30% of the cases. Dogs with less than five adult heartworms or all male heartworms will not have enough antigen to give a positive result, so there may be an occasional false negative result in dogs with early infections. Therefore, there must be at least five female worms present for the most common heartworm test to diagnose heartworm disease.
Blood test for microfilariae: A blood sample is examined under the microscope for the presence of microfilariae. If microfilariae are seen, the test is positive. The number of microfilariae seen gives us a general indication of the severity of the infection. However, the microfilariae are seen in greater numbers in the summer months and in the evening, so these variations must be considered. Approximately 20% of dogs do not test positive even though they have heartworms because of an acquired immunity to this stage of the heartworm. Because of this, the antigen test is the preferred test. Also, there is another blood parasite that is fairly common in dogs that can be hard to distinguish from heartworm microfilariae.
Blood chemistries: Complete blood counts and blood tests for kidney and liver function may give an indication of the presence of heartworm disease. These tests are also performed on dogs and cats diagnosed as heartworm infected to determine the function of the body’s organs prior to treatment.
Radiographs (X-rays): A radiograph of a dog with advanced heartworm disease may show heart enlargement and swelling of the large artery leading to the lungs from the heart. These signs are considered presumptive evidence of heartworm disease. Chest x-rays allow us to predict an increased possibility of complications related to treatment.
Electrocardiogram: An electrocardiogram (EKG or ECG) is a tracing of the electric currents generated by the heart. It is most useful to determine the presence of abnormal heart rhythms.
Echocardiography: In some severe cases of heartworm disease we may recommend referral for an echocardiogram, an ultrasonic examination of the heart.
How are dogs treated for heartworms?
There is some risk involved in treating dogs with heartworms, although fatalities are rare. In the past, the drug used to treat heartworms contained arsenic so toxic effects and reactions occurred more frequently. A newer drug is now available that does not have the toxic side-effects. We can now successfully treat more than 95% of dogs with heartworms.
Some dogs are diagnosed with advanced heartworm disease. This means that the heartworms have been present long enough to cause substantial damage to the heart, lungs, blood vessels, kidneys, and liver. A few of these cases will be so advanced that it will be safer to treat the organ damage rather than risk treatment to kill the heartworms. Dogs in this condition are not likely to live more than a few weeks or months.
Treatment to kill adult heartworms: An injectable drug to kill adult heartworms is given in two separate treatments one month apart. It kills the adult heartworms in the heart and adjacent vessels. In more serious infections, these injections may be divided and given thirty days apart.
Complete rest is essential after treatment: The adult worms die in a few days and start to decompose. As they break up, they are carried to the lungs, where they lodge in the small blood vessels and are eventually reabsorbed by the body. This can be a dangerous period so it is absolutely essential that the dog be kept quiet and not be allowed to exercise for one month following treatment. The first week after the injections is critical because the worms are dying. A cough is noticeable for seven to eight weeks after treatment in many heavily infected dogs.
Prompt treatment is essential if the dog has a significant reaction in the weeks following the initial treatment, although such reactions are rare. If a dog shows loss of appetite, shortness of breath, severe coughing, coughing up blood, fever, and/or depression, you should notify us. Response to antibiotics, cage rest, and supportive care and intravenous fluids is usually good in these cases.
Treatment to kill microfilaria: Approximately one month following treatment to kill the adults, the dog is returned to the hospital for administration of a drug to kill the baby heartworms or microfilariae, if present. Your dog needs to stay in the hospital for the day.
Other treatments: In dogs with severe heartworm disease, it may be necessary to treat them with antibiotics, special diets, diuretics to remove fluid accumulations, and drugs to improve heart function prior to treatment for the heartworms.
Dogs with severe heart disease may need lifetime treatment for the heart failure, even after the heartworms have been killed. This includes the use of diuretics, heart drugs, and special low salt, low protein diets.
Response to treatment: Dog owners are usually pleasantly surprised at the change in their dog following treatment for heartworms, especially if the dog had been showing signs of heartworm disease. The dog has a renewed vigor and vitality, improved appetite, and weight gain.
Are changes made in the treatment protocol for dogs that have severe heartworm disease?
Yes. The state of heart failure is treated as described above. Depending on the severity of the infection and organ damage present, we may or may not recommend treating the adult heartworms.
Can heartworms be treated in cats?
There is no drug approved for treating heartworms in cats. One of the drugs for treating dogs has been used in cats, but there are severe side-effects. Another problem is that when the heartworms die they pass through the pulmonary arteries to the lungs. This can result in sudden death. Thus, we have a dilemma when a cat is diagnosed with heartworms. One of two choices must be made:
1. Treat with the drug designed for dogs. However, this is a drug that has been shown to have side-effects in cats. These side-effects include acute pulmonary (lung) failure and death in a small percentage of cats.
2. Treat the symptoms of heartworm disease and hope the cat outlives the worms. Since heartworms live in a cat for about two years, several months of treatment are needed. When cats are in a crisis, they are treated with oxygen and corticosteroids (“cortisone”) to relieve the reaction occurring in the pulmonary arteries and lungs, and, if needed, drugs to remove fluid from the lungs (diuretics). When they are stable, they are treated continuously or periodically with corticosteroids. However, the threat of an acute crisis or sudden death always exists.
How can I prevent this from happening again?
It is essential to begin a heartworm prevention program to prevent future recurrence of heartworm infection. With the safe and affordable heart preventives available today, no pet should ever have to endure this dreaded disease.
Heartworm information is based on material written by Ernest E. Ward Jr., DVM.
©Copyright 2002 Lifelearn Inc. Used with permission under license.
Spaying and Neutering
Spaying and Neutering
At what age do female dogs/cats usually begin their “heat” cycles?
Depending on the breed and size, “heat”, or estrus, normally begins between 6 months and 1½ years of age. Smaller breeds generally begin at a younger age than large breeds. Estrual cycles tend to become seasonal and regular as the animal matures. Often mature females cycle twice a year, but not necessarily at exact six-month intervals.
Is it a good idea to have my pet “spayed” or “neutered”?
Yes! We recommend spaying or neutering your pet, and following are a few reasons why.
• Non-sterilized pets frequently develop undesirable behavior traits, such as fighting or roaming. In addition to owner inconvenience, these traits may endanger your pets’ life and longevity!
• Certain disease processes are less likely to occur in sterilized animals, such as mammary (breast) or testicular cancer.
• Surgical sterilization is the most consistent means of controlling the pet population problem.
When is the best time to have my female spayed?
 The optimum age to have a dog or cat spayed varies. For small breed dogs, we recommend spaying after five to six months of age in order to ensure that their baby teeth have fallen out. Large breed dogs ideally are spayed between 6 and 12 months. Cats are generally ready by five to six months of age. Please call our pet hospital to discuss the ideal time for spaying your dog.
The optimum age to have a dog or cat spayed varies. For small breed dogs, we recommend spaying after five to six months of age in order to ensure that their baby teeth have fallen out. Large breed dogs ideally are spayed between 6 and 12 months. Cats are generally ready by five to six months of age. Please call our pet hospital to discuss the ideal time for spaying your dog.
When should my male pet be neutered?
Again, for small breed dogs and cats we recommend five to six months of age, and for large breed dogs, between 6 and 12 months of age. Our veterinarians are happy to discuss the ideal time for neutering if you give us a call.
Vaccinations and Preventative Measures
Vaccinations and Preventative Measures
 When should a puppy or kitten be scheduled for vaccinations?
When should a puppy or kitten be scheduled for vaccinations?
Our veterinary clinic recommends beginning vaccinations at 6-8 weeks of age. Vaccinations given earlier than 6 weeks of age are ineffective due to the presence of maternal antibodies. Maternal antibodies are passed from mother to kitten through the milk, and provide immunity to young puppies and kittens until they can develop immunity of their own. Maternal antibodies interfere with vaccinations, rendering them ineffective; therefore, we do not recommend beginning vaccinations until 6-8 weeks of age, when animals begin to lose these antibodies.
How often should my pet be vaccinated?
Our veterinarians recommend the vaccinations be given every 3-4 weeks during the puppy and kitten series, then again at one year of age. After the one year booster, the distemper/parvo combination in dogs and the upper respiratory vaccination in cats are recommended every 3 years in our practice. There is a large body of evidence in veterinary medicine that suggests that these vaccinations are not necessary on a yearly basis. We’d be happy to discuss this further at your next visit.
Initial rabies vaccination is given after your pet reaches 3 – 4 months of age and is boostered one year later to ensure the effectiveness of the vaccine. Adult canine vaccinations (after that booster) are affected by the recent change in the City of Wichita’s ordinance which goes into effect on July 1, 2009. Rabies vaccines for adult dogs will be required every three years after that point, and in the intervening years, in lieu of the vaccination, the City requires a yearly examination by a veterinarian who certifies that the dog is healthy, signs off on the official license form, and issues a current rabies tag.
Our veterinarians will continue to vaccinate cats yearly for rabies. The difference is that a cat can develop, though rarely, a malignancy called a fibrosarcoma from the adjuvants (chemicals) added to the three year rabies vaccines. Dogs are not prone to fibrosarcoma development. Therefore, for the safety of our feline patients, we will still recommend a non-adjuvanted one-year rabies vaccine for cats.
Canine Leptospirosis Vaccine
Leptospirosis is a bacterial disease of dogs and other mammals that particularly affects the liver or kidneys. Leptospira bacteria are carried mainly by rats and other rodents along with wildlife such as raccoons and opossums but can affect almost any mammalian species, including people. The fact that humans can contract Lepto (for short) from these animal sources (but especially from their own pets), makes it a zoological disease. Lepto is spread through the urine of an infected animal and is ingested by other animals through, for example, contaminated water sources, areas where rodents and/or raccoons congregate, and the like. A dog that swims in contaminated water can even become infected through its skin if the skin is damaged or thin. Signs of infection may be extreme lethargy, lack of desire to eat, and perhaps vomiting. Fever may or may not be present, but other signs include diarrhea, excessive drinking, and abdominal discomfort. Of course, many of these symptoms are shared with other diseases and disorders, but Leptospirosis is a possibility if one factors in the dog’s activities, habits, and environmental exposure. Effective treatment consists of a course of antibiotics and concurrent intensive hospital care which are especially effective if the disease is caught early and treatment is begun immediately. We have seen an increased incidence of this disease in our practice and, therefore, we are strongly recommending the Leptospirosis vaccine to be administered to our canine patients as a preventive measure.
 Are there any side-effects to vaccinations?
Are there any side-effects to vaccinations?
Vaccinations are generally very safe, but reactions can occur. Occasionally, a pet can experience mild lethargy, vomiting, or diarrhea after a vaccine. Local reactions can occur and can appear as painful or nonpainful knots in the area of vaccination, small bumps on the skin, or a swollen muzzle/face. Severe vaccination reactions are rare, but can be quite serious. If you are concerned about your pet post-vaccination, please call us immediately. We may recommend your pet be seen by a veterinarian.
Health insurance options for your pet.
It’s no secret that owning a pet isn’t cheap. They require medical attention, just like we do, and it can be a struggle sometimes to pay for it. Pet health insurance is becoming increasingly popular because it allows pet owners to be able to afford veterinary services for their pets that they might otherwise have not been able to. Our veterinarians and staff think pet health insurance is a great idea. Listed below are links to websites of pet health insurance companies that our clients have found valuable.
